Success rate has improved but cost and high processing power are concerns
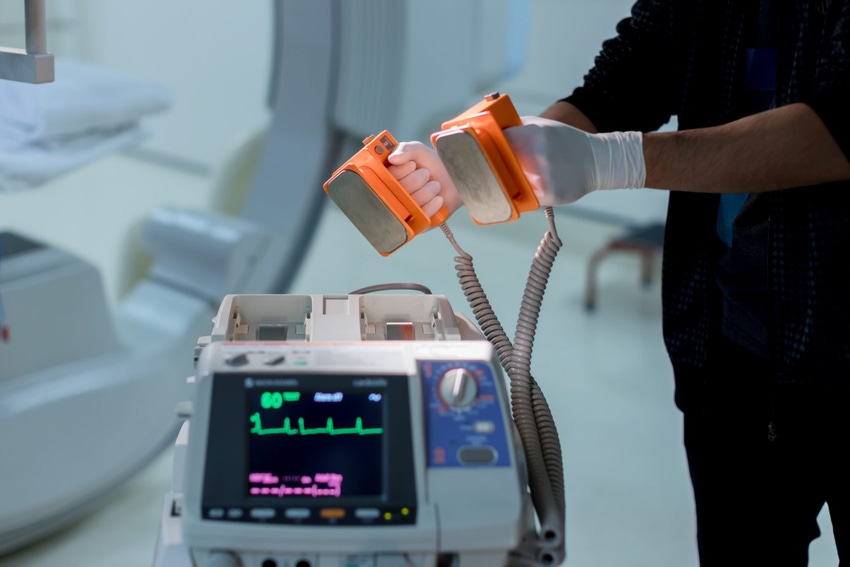
Defibrillators are used to deliver electrical currents to the heart as treatment for cardiac arrest that can potentially be fatal. AI is making a big impact on how defibrillators can work more efficiently, with machine learning algorithms becoming increasingly accurate with life-saving treatments, according to a recent paper.
Automated external defibrillators (AEDs) and implantable cardioverter defibrillators (ICDs) leverage shock-advice algorithms to distinguish echocardiogram tracings. The data determines whether rhythms are deemed “shockable” or “non-shockable” to decide whether defibrillation is necessary for treatment.
AI can also be used to diagnose the causes of heart attacks, classify heart rhythms without interrupting cardiopulmonary resuscitation (CPR), and predict the success of defibrillation, according to “Role of artificial intelligence in defibrillators: a narrative review,” by researchers from U.K. hospitals and universities.
While the success rate has improved, concerns around cost and high processing power remain a challenge.
How machine learning is implemented in medical applications has evolved over recent years. Currently, supervised machine learning models are still necessary for defibrillator applications. Deep learning replicates the brain’s neural networks with artificial neural networks (ANN), which contain layers of nodes that process input data.
AI can be leveraged for standard ECG analysis. Convolutional neural networks (CNNs) are a sub-category of ANN, which uses high-level features from the raw data. This method has been used in medical imaging and ECG analysis but can also be used to evaluate multiple dimensions in data sets. In one model, ECG interpretation by CNN was more accurate than human cardiologists but automated ECG analysis is still not used extensively.
Smart watches, like the Apple Watch, and other wearable technology has become more widely used, especially with the capability to conduct automated single-lead ECGs to detect atrial fibrillation.
In one study, the Kardia Band (KB) algorithm, used in Apple Watches, wasn’t as accurate as clinicians’ diagnosis. The algorithm wasn’t able to interpret more than half the ECG and KB recordings. Physician oversight is still necessary for the most accurate diagnosis.
In addition, AI can be used as a screen for early pulmonary hypertension and asymptomatic left ventricular dysfunction. Mayo Clinic used data from almost 45,000 patients to teach a CNN to identify asymptomatic left ventricular dysfunction. The results were promising, showing a positive AI screen predicted a four times greater risk of developing ventricular dysfunction than the patients who didn’t use the screen.
AI can also evaluate when to stop CPR and optimize shock delivery. It can also reduce the number of unnecessary shocks, which will improve the patient’s quality of life. Future plans include creating a robust dataset of ECGs for building and testing algorithms to compare technologies.
About the Author(s)
You May Also Like
.png?width=100&auto=webp&quality=80&disable=upscale)
.png?width=400&auto=webp&quality=80&disable=upscale)
.png?width=700&auto=webp&quality=80&disable=upscale)
.png?width=700&auto=webp&quality=80&disable=upscale)

.png?width=300&auto=webp&quality=80&disable=upscale)
.png?width=300&auto=webp&quality=80&disable=upscale)
.png?width=300&auto=webp&quality=80&disable=upscale)
